Opioid Addiction: Understanding the Crisis and Finding Help
The opioid epidemic has claimed over 500,000 lives in the U.S. Understand how opioid addiction develops and the life-saving treatments available.

The Scope of the Opioid Epidemic
Opioid addiction has killed more than 500,000 Americans since 1999. The crisis evolved through three distinct waves: an increase in prescription opioid deaths beginning in the late 1990s, a surge in heroin deaths starting in 2010, and a catastrophic rise in synthetic opioid (fentanyl) deaths beginning in 2013.
Today, synthetic opioids account for over 73% of all opioid overdose deaths. The crisis affects every demographic, geographic region, and socioeconomic group in the country.
How Opioids Work in the Brain
Opioids bind to mu-opioid receptors in the brain, spinal cord, and gut. This binding triggers dopamine release in the reward center, producing pain relief and euphoria. With repeated use, the brain reduces its natural endorphin production and increases opioid receptor density, creating physical dependence.
Tolerance develops as the brain adapts to opioids, requiring higher doses for the same effect. This escalation drives many people from prescription pills to cheaper, more potent alternatives like heroin and illicitly manufactured fentanyl.
Commonly Abused Opioids
- Prescription: oxycodone, hydrocodone, morphine, codeine, tramadol
- Illicit: heroin, illicitly manufactured fentanyl and its analogs
- Combined products: Vicodin, Percocet, OxyContin
Signs of Opioid Addiction
- Constricted (pinpoint) pupils
- Drowsiness and nodding off at inappropriate times
- Slurred speech and impaired coordination
- Frequent flu-like symptoms (withdrawal beginning)
- Doctor shopping or obtaining opioids from multiple sources
- Social withdrawal and secrecy about activities
- Financial problems or missing valuables at home
- Needle marks (if injecting) or nasal damage (if snorting)
Opioid Withdrawal
Opioid withdrawal begins 8-24 hours after the last dose (for short-acting opioids) and causes intense discomfort:
- Severe muscle and bone pain
- Diarrhea, nausea, and vomiting
- Insomnia and restless legs
- Cold sweats, goosebumps, and runny nose
- Intense cravings
- Anxiety, agitation, and irritability
Withdrawal is rarely fatal but extremely uncomfortable. Fear of withdrawal keeps many people using opioids even when they want to stop.
Medication-Assisted Treatment Saves Lives
MAT is the gold standard for opioid use disorder, combining FDA-approved medications with behavioral therapy:
- Buprenorphine (Suboxone, Sublocade) is a partial opioid agonist that reduces cravings and withdrawal without producing a full high. It is prescribed in office-based settings.
- Methadone is a full opioid agonist dispensed through certified clinics. It stabilizes brain chemistry and blocks the effects of other opioids.
- Naltrexone (Vivitrol) is an opioid antagonist that completely blocks opioid effects. Available as a monthly injection after full detoxification.
Research published in the New England Journal of Medicine shows that MAT reduces opioid overdose deaths by more than 50% and significantly improves treatment retention compared to behavioral therapy alone.
Behavioral Therapies
Medications work best when combined with counseling. Effective behavioral approaches include CBT, contingency management, motivational interviewing, and group therapy. Family involvement improves outcomes, especially for adolescents and young adults.
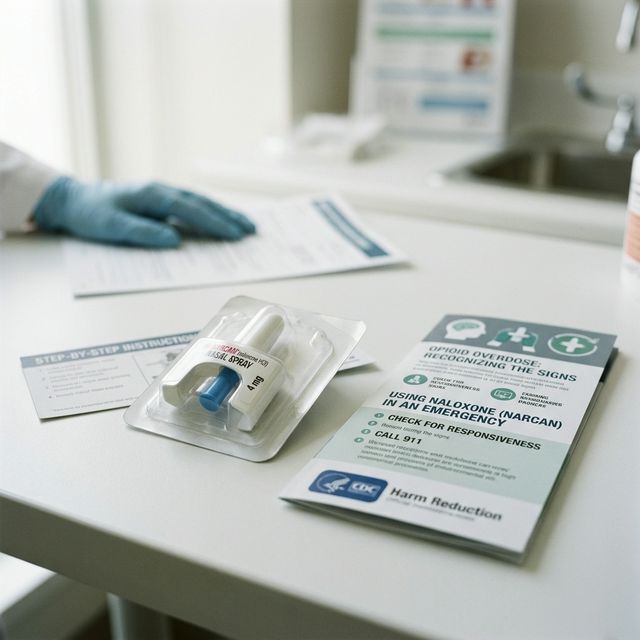
Naloxone Is Essential
Anyone with opioid use disorder, or anyone in their life, should carry naloxone. This medication reverses opioid overdose within minutes and is available without a prescription at most pharmacies. It has no abuse potential and no effect on people who have not used opioids.
Frequently Asked Questions
- Is medication-assisted treatment just replacing one addiction with another?
- No. MAT medications like buprenorphine and methadone are evidence-based treatments that stabilize brain chemistry, reduce cravings, and prevent overdose. They allow people to function normally, maintain employment, and engage in therapy. Major medical organizations including the WHO endorse MAT as the standard of care.
- How does someone go from prescription pills to heroin?
- As tolerance builds, prescription opioids become harder and more expensive to obtain. Heroin produces similar effects at a fraction of the cost. NIDA reports that about 80% of heroin users first misused prescription opioids. However, the vast majority of prescription opioid users do not transition to heroin.
- Can you die from opioid withdrawal?
- Opioid withdrawal is rarely fatal on its own in otherwise healthy adults. However, severe dehydration from vomiting and diarrhea poses risks if untreated. Medical supervision during withdrawal is strongly recommended, especially for people with other health conditions.
- How long does opioid addiction treatment take?
- NIDA recommends a minimum of 90 days in treatment. Many experts recommend at least 1-2 years on MAT medications, and some patients benefit from indefinite maintenance. Treatment duration should be individualized based on response and risk factors.
Sources & References
This article is informed by research and data from the following authoritative sources:
This article is for educational purposes only and should not be considered medical advice. Always consult a qualified healthcare provider before making decisions about addiction treatment. If you or someone you know is in crisis, call SAMHSA's National Helpline: 1-800-662-4357 (free, confidential, 24/7).