How Washington Spends Opioid Settlement Cash in the Tri-Cities
How Washington Spends Opioid Settlement Cash in the Tri-Cities Tri-Cities leaders just received a new wave of Washington opioid settlement dollars, and the…
How Washington Spends Opioid Settlement Cash in the Tri-Cities
Tri-Cities leaders just received a new wave of Washington opioid settlement dollars, and the spending fight has already started. The stakes are blunt: overdose deaths keep climbing, families are exhausted, and residents want to see visible change. Washington opioid settlement money should fund treatment beds, street outreach, and proven harm reduction tools, yet local governments often bury funds in spreadsheets. You deserve to know who is getting the cash, what results to expect, and how to press for transparency. This is not abstract policy. It is your neighbor’s ability to find detox tonight, your library’s safety, and your county’s capacity to move faster than fentanyl.
What matters right now
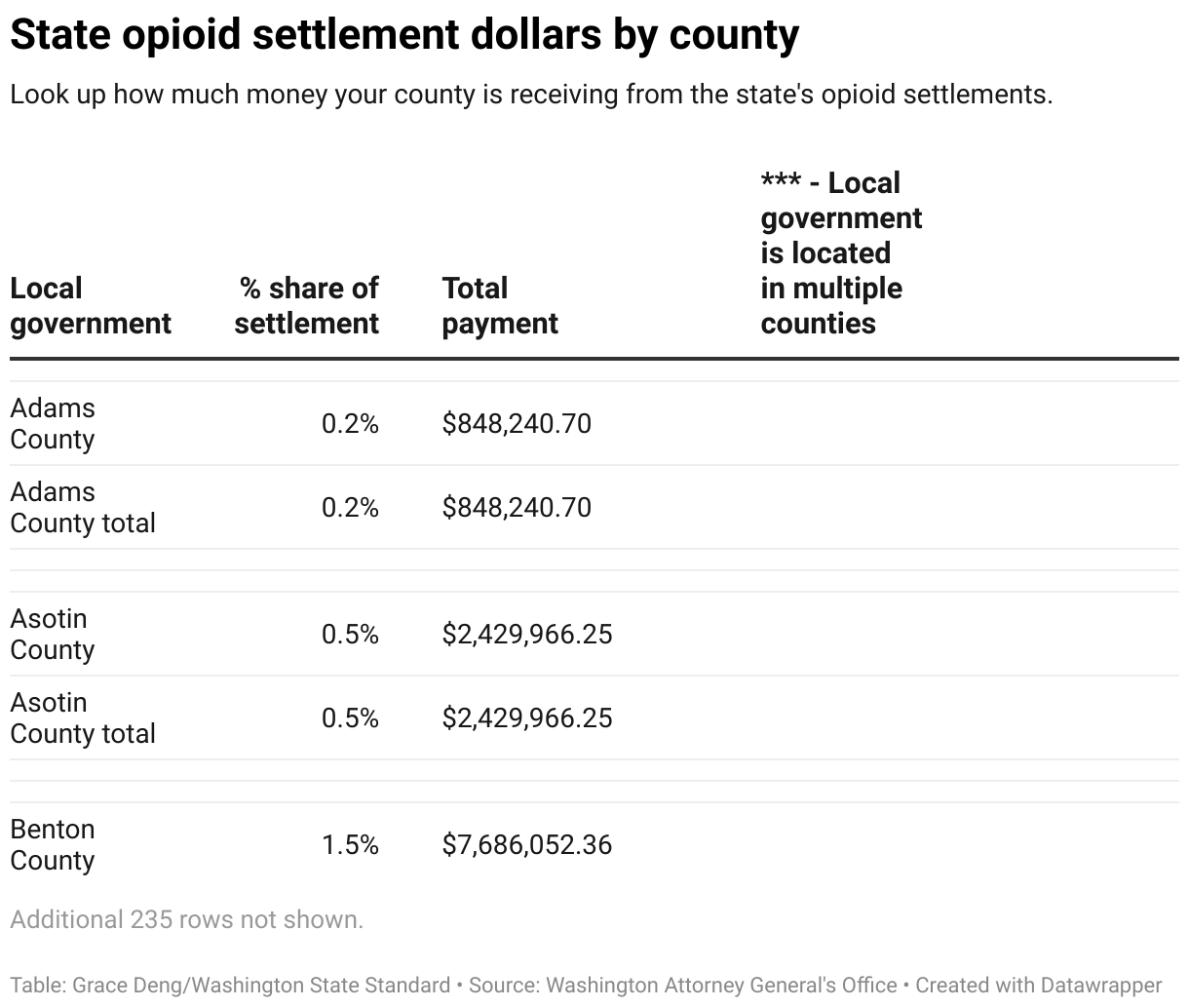
- Roughly $1.1 billion in Washington opioid settlement payments will be spread over 17 years.
- Benton and Franklin counties will split millions, but allocations differ by population and overdose rates.
- Spending must align with Exhibit E of the state agreement, favoring treatment, housing, and prevention.
- Public dashboards and quarterly reports are the quickest way to prove impact.
- Residents can shape budgets during county commission and city council hearings.
Washington opioid settlement spending priorities
Counties want quick wins, but the agreement puts guardrails around the money. Core buckets include medication-assisted treatment (MAT), overdose reversal distribution, supportive housing, and youth prevention. Think of it like setting a baseball lineup: you need reliable hitters at the top, not a random bench crowd. Leading with naloxone distribution and low-barrier clinics keeps people alive long enough to reach treatment. Layer in housing supports so progress does not evaporate overnight.
Look, the political temptation is to patch old budgets. Resist that. Push for projects that add capacity: more detox beds, mobile crisis teams, and extended clinic hours. Who gets held accountable if the funds vanish into bureaucracy?
Practical moves for local officials
- Publish a line-item plan that maps each dollar to a state-approved category.
- Commit to outcome targets: reduced overdose calls, faster clinic intake, and more people completing MAT.
- Fund community partners that already serve the hardest-hit blocks rather than spinning up new agencies.
- Schedule public check-ins every quarter with real numbers, not slogans.
Transparency beats slogans. If a county cannot show a public ledger, it does not deserve the next payment.
This is a stress test for public trust.
Tracking Washington opioid settlement results
Residents can track the money with the same focus you’d use on a household budget. Start with the state’s Opioid Abatement Council site, then check county commission packets for contract details. And demand machine-readable data (yes, that means better dashboards) instead of glossy PDFs. The goal is simple: connect dollars to fewer funerals and fewer 911 calls.
Questions to press at hearings
- How much went to direct services versus administrative overhead?
- Which neighborhoods receive outreach, and how were they chosen?
- What metrics will trigger shifting funds if a program underperforms?
- Are law enforcement and public health coordinating on overdose mapping?
One strong line of oversight: require vendors to publish monthly outcomes before invoices get paid. No data, no check. It is blunt, but it keeps the incentives aligned with public safety.
Tri-Cities examples worth copying
Early pilots in Kennewick and Pasco point to what works. Mobile response vans that pair a nurse with a peer counselor cut response times and lighten police workloads. School-based prevention led by local counselors resonates more than canned curricula. Shelter partnerships that reserve beds for people leaving detox reduce the bounce-back to the street. Each of these efforts shares a pattern: small teams, clear metrics, rapid iteration. Like a good kitchen line, everyone knows the next move.
What could derail the Washington opioid settlement plan
Three risks keep popping up. First, cities might chase shiny projects that do little for overdose numbers. Second, contract management can lag, slowing the release of funds. Third, community groups sometimes get tangled in compliance paperwork. The fixes are straightforward: cap administrative spend, pre-negotiate templated contracts, and offer technical assistance to smaller providers so they are not drowned in forms. But will leaders keep the pace once cameras leave?
What to watch next
Expect another reporting cycle before winter. If the numbers do not show more people in treatment and more naloxone on the street, demand course corrections. The settlement lasts 17 years, but urgency cannot wait that long. Stay in the room, ask for the ledger, and keep the pressure on until the Tri-Cities see fewer obituaries and more recovery stories.
This article is for educational purposes only and should not be considered medical advice. Always consult a qualified healthcare provider before making decisions about addiction treatment. If you or someone you know is in crisis, call SAMHSA's National Helpline: 1-800-662-4357 (free, confidential, 24/7).