Opioid Overdose: Signs, Risks, and Fast Action
Opioid Overdose: Signs, Risks, and Fast Action An opioid overdose can turn fatal in minutes, and many people still miss the early signs or wait too long to…
Opioid Overdose: Signs, Risks, and Fast Action
An opioid overdose can turn fatal in minutes, and many people still miss the early signs or wait too long to act. That delay matters. Opioids such as heroin, morphine, codeine, methadone, fentanyl, and tramadol can slow breathing until the brain and body shut down. The World Health Organization says opioid overdose is a major public health problem, tied to both illicit drug use and prescribed medicines. You might be worried about your own risk, a family member, or someone in treatment who seems stable but is still vulnerable. Fair concern. The danger often rises after reduced tolerance, mixed drug use, or poor access to emergency help. If you know what opioid overdose looks like, and what lowers the odds, you are in a much stronger position to respond fast and possibly save a life.
What matters most
- Slow or stopped breathing is the most dangerous sign of opioid overdose.
- Risk jumps when opioids are mixed with alcohol, benzodiazepines, or other sedating drugs.
- Naloxone can reverse opioid overdose and should be available to people at risk and those around them.
- Lower tolerance after detox, release from prison, or a break in use can make a previously familiar dose deadly.
What is an opioid overdose?
An opioid overdose happens when opioids overwhelm the parts of the brain that control breathing. Breathing slows, becomes shallow, or stops. Without oxygen, a person can lose consciousness, suffer brain injury, or die.
WHO identifies opioids as substances that act on opioid receptors to reduce pain. That group includes prescription medicines and illegal drugs. Different names, same core risk.
Opioid overdose is often a breathing emergency before it is anything else. If breathing drops, time gets very short.
Opioid overdose signs you should not brush off
Some signs are easy to spot. Others are subtle at first, which is why people freeze or second-guess themselves. But if you are asking, “Is this serious?” the safer move is to treat it like an emergency.
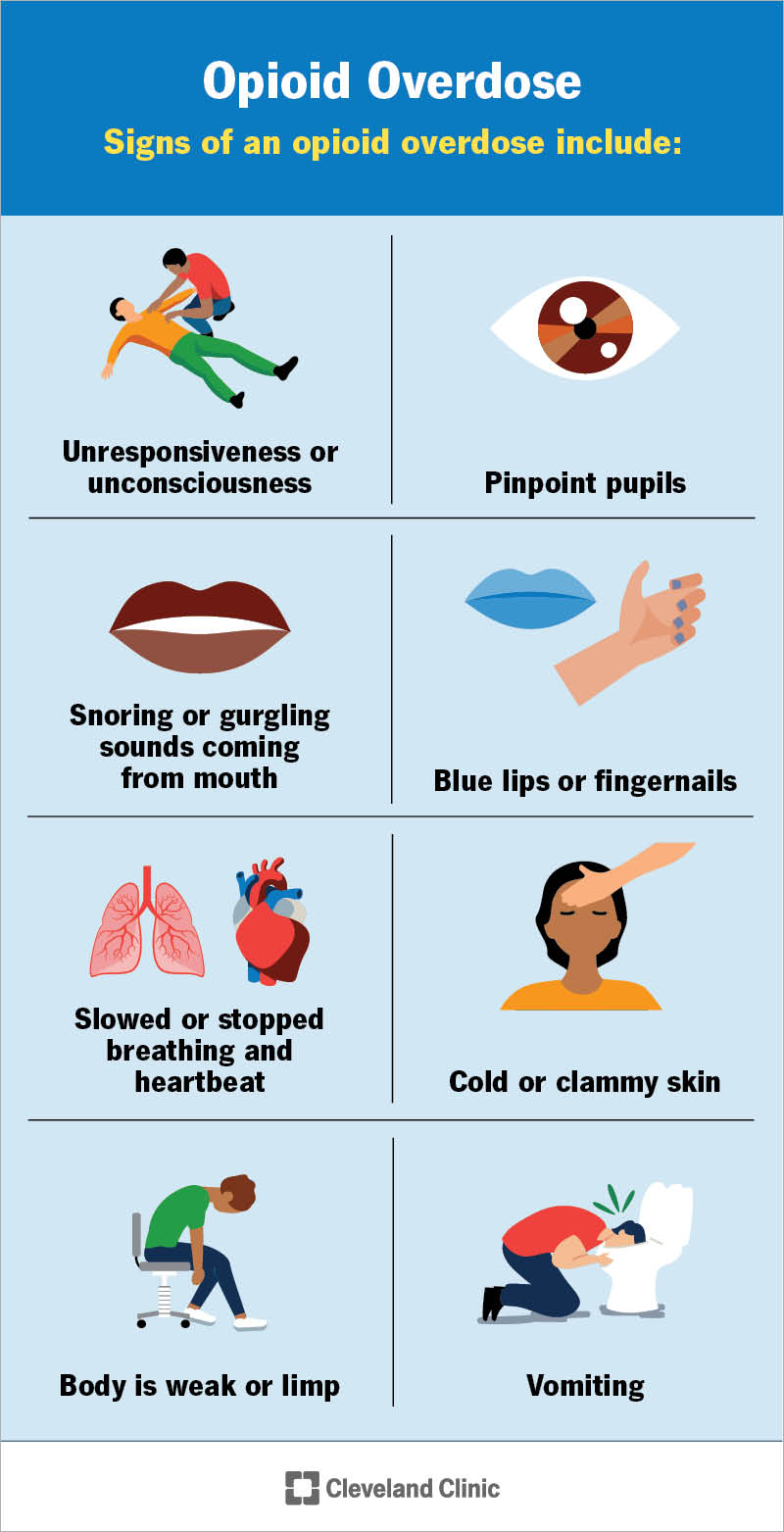
Common opioid overdose signs
- Very slow breathing or no breathing
- Pinpoint pupils
- Unconsciousness or inability to wake the person
- Blue or purple lips and fingernails
- Snoring, choking, or gurgling sounds
- Limp body
- Pale, cold, or clammy skin
That gurgling sound matters.
People sometimes mistake it for sleep, especially if the person used drugs before and “slept it off” in the past. Honestly, that is one of the most dangerous assumptions in this space. An opioid overdose can look quiet, almost still, right before it turns catastrophic.
Who faces the highest opioid overdose risk?
Not everyone who uses opioids faces the same odds. WHO points to several groups at higher risk, and the pattern is clear. Overdose tends to hit hardest when tolerance, access, and drug mixing all collide.
Situations that raise opioid overdose risk
- Using high doses of opioids, whether prescribed or nonmedical.
- Mixing opioids with alcohol, benzodiazepines, or other sedatives.
- Returning to opioid use after a break, such as after detox, treatment, jail, prison, or hospitalization.
- Having health conditions like HIV, liver disease, lung disease, or depression.
- Using opioids alone, when nobody is there to call for help or give naloxone.
Reduced tolerance is a brutal trap. A dose that once felt routine can become lethal after even a short period of abstinence. Think of it like an athlete trying to lift last season’s max after months off. The memory is there. The body is not.
Why fentanyl and drug mixing change the equation
Some opioids are far more potent than others. Fentanyl and related synthetic opioids have changed overdose patterns in many countries because tiny amounts can have a large effect. That makes street drugs far less predictable, especially when people do not know fentanyl is present.
And then there is mixing. WHO warns that combining opioids with sedating substances, especially benzodiazepines and alcohol, raises the risk of fatal respiratory depression. This is where a lot of public messaging falls short. People hear “opioids” and think only of heroin. But prescription pills plus alcohol can be just as deadly.
What to do during an opioid overdose
If you suspect an opioid overdose, act fast. Do not wait for certainty. A quick response can keep oxygen flowing until emergency care arrives.
Fast steps that can save a life
- Try to wake the person. Shout their name and rub your knuckles firmly on the center of their chest.
- Call emergency services right away.
- Give naloxone if you have it, following the product instructions.
- Support breathing if you are trained to do so.
- Place the person on their side in the recovery position if they are breathing on their own.
- Stay with them until help arrives.
Naloxone is a medicine that reverses the effects of opioids for a limited time. WHO supports broad access to naloxone for people likely to witness an overdose, including friends, family, and peers. That stance makes sense. Waiting for a clinician to be the only responder is like keeping fire extinguishers locked in city hall.
How naloxone fits into opioid overdose prevention
Naloxone is one of the clearest harm reduction tools available. It can be given by injection or nasal spray, depending on the product and setting. It is not a substitute for emergency care, because the person can slip back into overdose after it wears off (especially with long-acting opioids), but it buys precious time.
Look, availability matters. A naloxone policy that exists on paper but does not reach households, shelters, treatment programs, and community workers will not move the needle much.
Who should have naloxone nearby?
- People who use opioids, including prescription opioids
- People with a history of opioid use disorder
- Anyone leaving detox, residential treatment, jail, or prison
- Household members and close friends of a person at risk
- Staff in services that support people who use drugs
Practical ways to lower opioid overdose risk
You cannot reduce every risk, but you can cut several of the biggest ones. The smart approach is to stack protections, not rely on one fix.
- Avoid mixing opioids with alcohol, benzodiazepines, or other sedating drugs.
- Use extra caution after a period of not using, because tolerance may be lower.
- Keep naloxone on hand and make sure people around you know where it is.
- Do not use alone if overdose risk is present.
- Follow prescribing directions closely if you use opioid pain medicines.
- Seek treatment for opioid use disorder, including evidence-based options such as opioid agonist maintenance treatment where available.
One more point matters here. WHO supports treatment access that includes medication-based care, because prevention is not only about the crisis moment. It is also about reducing the odds of that moment happening again.
What families should know about opioid overdose
Families often spot risk changes before anyone else. A loved one returns home after treatment. A person restarts use after release from custody. Someone mixes pills with alcohol and insists they are fine. You do not need perfect knowledge to take sensible steps.
Ask direct questions. Keep naloxone in the home. Learn the overdose signs. And if the person is in treatment or recovery, talk openly about reduced tolerance after time away from opioids. Why pretend this is too awkward to say out loud when the stakes are this high?
Where the response needs to go next
Opioid overdose is not a mystery. The signs are known. The risk factors are well documented. Naloxone works, and broader access saves lives, according to WHO. The real test is whether health systems, policymakers, and families treat overdose response as basic readiness instead of a niche issue. If you are close to this risk, the next smart move is simple. Learn the signs, carry naloxone, and make sure the people around you know how to use it.
This article is for educational purposes only and should not be considered medical advice. Always consult a qualified healthcare provider before making decisions about addiction treatment. If you or someone you know is in crisis, call SAMHSA's National Helpline: 1-800-662-4357 (free, confidential, 24/7).