Family Mental Health Interventions That Actually Help
Family Mental Health Interventions That Actually Help If your family is trying to help someone with a mental health or substance use problem, you may feel…
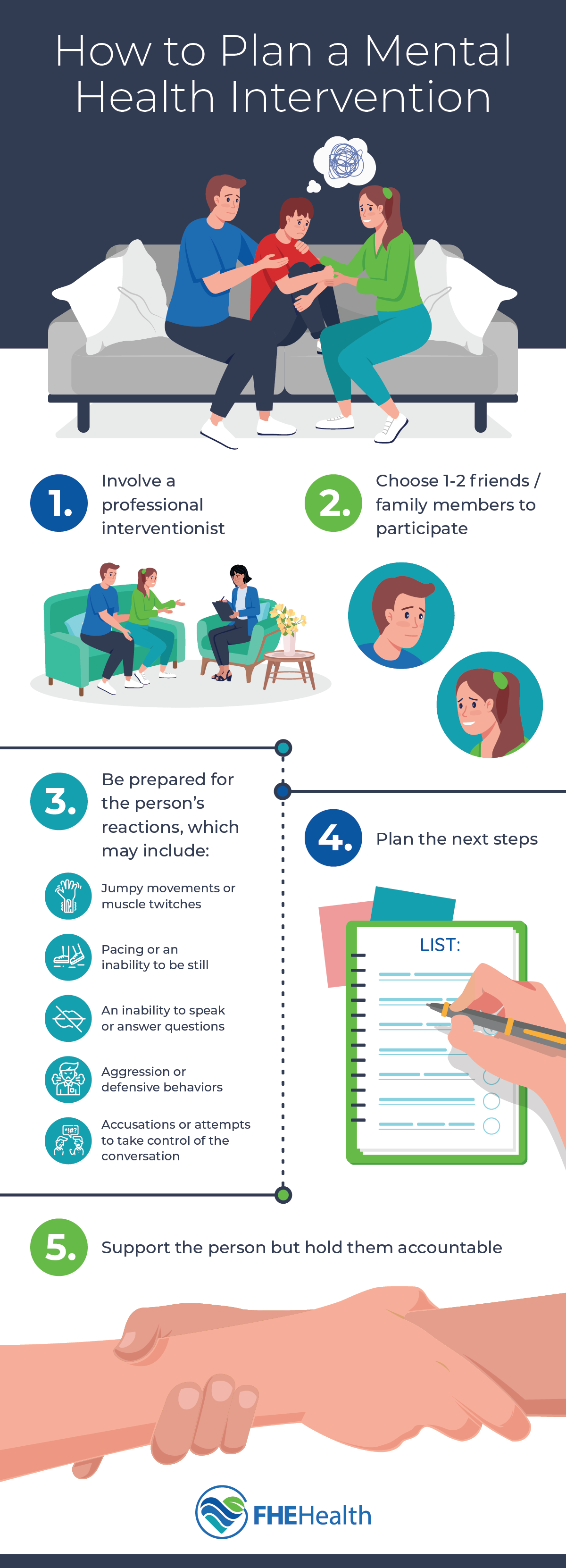
Family Mental Health Interventions That Actually Help
If your family is trying to help someone with a mental health or substance use problem, you may feel stuck. One day you want to protect them. The next day you are setting limits, then second-guessing yourself. That confusion can drag on for months or years. Family mental health interventions matter because the usual pattern, waiting for a crisis or hoping a person will ask for help on their own, often fails. Families need a clearer plan. They also need support for themselves, not just for the loved one in pain. A recent feature on Reflection Family Interventions points to a shift that deserves attention. The work is less about confrontation and more about structure, safety, and recovery for the whole family. That is a smarter model, and honestly, it is overdue.
What stands out
- Family mental health interventions work best when they support the whole household, not only the identified person.
- The strongest approach replaces blame with boundaries, planning, and steady follow-through.
- Mental health and addiction often overlap, so families need guidance that addresses both.
- Help should start before a crisis hits, not after things fall apart.
Why family mental health interventions are changing
Older ideas about intervention often centered on one dramatic moment. Get everyone in a room, confront the person, and push for treatment. That model still shows up in pop culture, but real life is messier.
The ABC15 feature on Reflection Family Interventions highlights a broader approach. The focus is on how families can support mental health and recovery in a more informed way. That means looking at communication, limits, treatment options, and the family system itself. It is closer to repairing a house foundation than painting over a cracked wall.
Families often need help learning how to respond in ways that support recovery instead of feeding chaos.
And that shift makes sense. The Substance Abuse and Mental Health Services Administration, or SAMHSA, has long stressed the value of family involvement in recovery support. The National Institute on Drug Abuse also notes that addiction affects families and that family-based approaches can improve treatment engagement and outcomes.
What family mental health interventions actually look like
Look, this is not about finding the perfect script. It is about building a plan that lowers harm and raises the odds of treatment.
In practice, family mental health interventions often include assessment, coaching, structured conversations, treatment coordination, and post-placement support. Some models also prepare families for resistance, relapse, or partial progress. Because yes, progress is often uneven.
Core parts of a solid intervention plan
- Clarify the problem. Is the main issue untreated depression, trauma, alcohol use, opioid misuse, or a mix of several factors?
- Map the family pattern. Who rescues, who withdraws, who escalates, and who keeps secrets?
- Set non-negotiable boundaries. These might involve money, housing, transportation, or behavior in the home.
- Prepare treatment options. That can include inpatient care, outpatient therapy, psychiatric evaluation, or dual-diagnosis treatment.
- Support the family too. Coaching, counseling, and education help relatives stop reacting from panic.
That last point gets ignored far too often.
Why the whole-family approach works better
A person in crisis does not exist in a vacuum. Their choices affect the family, and the family response affects them right back. That does not mean the family caused the illness or addiction. It means the system around the person can either steady the situation or make it worse.
Think of it like a basketball team. One player may be injured, but the whole offense changes to compensate. If everyone keeps improvising, the game gets sloppy fast. Families do the same thing under stress. They cover, absorb, argue, and adapt, often without realizing the pattern has become part of the problem.
A more effective intervention helps each person understand their role. It asks hard questions. Are you helping, or are you shielding someone from consequences? Are your rules clear, or do they change every week? What happens when the person says no?
Family mental health interventions and addiction recovery often overlap
This is where many families get blindsided. A loved one may seem to have an addiction issue, but untreated anxiety, bipolar disorder, trauma, or major depression may be driving part of the behavior. Or the reverse. A mental health crisis may be worsened by substance use.
That overlap is common. According to the National Institute of Mental Health and SAMHSA, co-occurring mental health and substance use disorders are widespread and often require integrated care. Families should be wary of one-size-fits-all advice, especially advice that treats addiction and mental health as separate silos.
Honestly, if a provider ignores one side of that equation, keep looking.
What families can do right now
You do not need to wait for a final blowup to make better decisions. Early action usually gives families more options, and more control.
Start here
- Document patterns. Write down incidents, symptoms, substance use concerns, and safety issues.
- Stop making secret side deals. Mixed messages from relatives weaken boundaries fast.
- Get a professional read. An intervention specialist, therapist, or addiction counselor can help sort urgency from panic.
- Decide your limits. Be specific about what you will and will not fund, allow, or excuse.
- Build a treatment path. Identify real options before the conversation happens.
But here is the hard part. A family plan only works if people stick to it after the emotional meeting is over.
What to watch for in an intervention service
Not every service offers the same depth. Some focus only on the event itself. Others work with the family before, during, and after treatment entry. The second model is usually stronger because recovery is not a one-day performance.
Ask direct questions:
- Do they have experience with both mental health and substance use cases?
- Do they coach the family, or only stage the intervention?
- Do they help with treatment placement and follow-up?
- How do they handle safety risks, refusal, or relapse?
- What is their view on family boundaries and long-term support?
A good provider should give plain answers, not vague sales talk.
The real test comes after treatment starts
Getting someone to accept help is only the opening move. The deeper work starts after admission, or after an outpatient plan begins. Families often expect relief at that point, then run into a new set of problems. Guilt, resentment, old habits, and pressure to return to the old normal.
That is why family support matters so much during recovery. Counseling, peer groups, and structured education can help relatives stop swinging between rescue and anger. Even small shifts count (like refusing to bankroll destructive behavior while still offering rides to therapy or support group meetings).
What is the goal, really? It is not control. It is a healthier family system that can support recovery without collapsing under it.
Where this approach is headed
The reporting on Reflection Family Interventions points to something bigger than one company. Families are starting to reject the old all-or-nothing script. They want a model that respects mental health, recognizes addiction, and gives relatives practical tools instead of guilt.
That is the right direction. If more families treat intervention as a process, not a showdown, outcomes should improve. And if providers keep putting family education at the center, the next generation of recovery support may look a lot more honest, and a lot more useful.
This article is for educational purposes only and should not be considered medical advice. Always consult a qualified healthcare provider before making decisions about addiction treatment. If you or someone you know is in crisis, call SAMHSA's National Helpline: 1-800-662-4357 (free, confidential, 24/7).